- Adrenal glands
- Adrenalectomy
- Indications of Adrenalectomy
- Symptoms
- Diagnosis
- Treatment Options
- Benefits and Drawbacks
- Complications
What are Adrenal Glands?
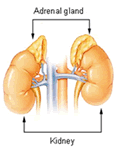 Adrenal glands are a part of our endocrine system. They are two small organs, located one above each kidney. They are triangular in shape and about the size of a thumb. These glands produce hormones which are involved in control of blood pressure, chemical levels in the blood, water use in the body, glucose usage, and the "fight or flight" reaction during times of stress. These adrenal-produced hormones include cortisol, aldosterone, the adrenaline hormones and a small fraction of the body's sex hormones (oestrogen and androgens).
Adrenal glands are a part of our endocrine system. They are two small organs, located one above each kidney. They are triangular in shape and about the size of a thumb. These glands produce hormones which are involved in control of blood pressure, chemical levels in the blood, water use in the body, glucose usage, and the "fight or flight" reaction during times of stress. These adrenal-produced hormones include cortisol, aldosterone, the adrenaline hormones and a small fraction of the body's sex hormones (oestrogen and androgens).
What is Adrenalectomy?
The procedure of removal of an adrenal gland is called an Adrenalectomy. The adrenal gland may be removed on one side or both sides at the time of surgery depending on the nature of disease. An Adrenalectomy is the surgical removal and this procedure can be performed using an open incision or laparoscopic technique.
What are the indications of Adrenalectomy?
Diseases of the adrenal gland are relatively rare. The most common reason that a patient may need to have the adrenal gland removed is because of tumour within adrenal gland. Most of these tumours are small and not cancers. They are known as benign growths that can usually be removed with surgery. Removal of the adrenal gland may also be required for certain tumours even if they aren't producing excess hormones, such as very large tumours or if there is a suspicion that the tumour could be a cancer, or sometimes referred to as malignant. Fortunately, malignant adrenal tumours are rare. An adrenal mass or tumour is sometimes found by chance when a patient gets an X-ray study to evaluate another problem. Occasionally, Adrenalectomy may be recommended when hormones produced by the adrenal glands aggravate another condition such as breast cancer. Let us see the common indications for removal of the adrenal gland are the following:
- Benign adrenal tumours such as Cushing disease and Cohn syndrome
- Pheochromocytoma
- Metastatic disease (spread) from lung, breast and other cancers. This is an uncommon reason for removal of the adrenal gland. The adrenal gland would only be considered for removal in metastatic disease if this were the only site of metastatic disease
- Adrenal mass (enlargement) of uncertain origin. If the adrenal gland is more than 4cm large then there is a higher risk of cancer than a smaller mass.
Patients with adrenal gland problems may have a variety of symptoms related to excess hormone production by the abnormal gland. Adrenal tumours associated with excess hormone production include pheochromocytomas, aldosterone-producing tumours, and cortisol-producing tumours. Some of these tumours and their typical features are given below.
- Pheochromocytomas produce excess hormones that can cause very high blood pressure and periodic spells characterized by severe headaches, excessive sweating, anxiety, palpitations, and rapid heart rate that may last from a few seconds to several minutes.
- Aldosterone producing tumours cause high blood pressure and low serum (blood) potassium levels. In some patients this may result in symptoms of weakness, fatigue, and frequent urination.
- Cortisol producing tumours cause a syndrome termed Cushing's syndrome that can be characterized by obesity (especially of the face and trunk), high blood sugar, high blood pressure, menstrual irregularities, fragile skin, and prominent stretch marks. Most cases of Cushing's syndrome, however, are caused by small pituitary tumours and are not treated by adrenal gland removal. Overall, adrenal tumours account for about 20% of cases of Cushing's syndrome.
- An incidentally found mass in the adrenal may be any of the above types of tumours, or may produce no hormones at all. Most incidentally found adrenal masses do not make excess hormones, cause no symptoms, are benign, and do not need to be removed. Surgical removal of incidentally discovered adrenal tumours is indicated only if:
- The tumour is found to make excess hormones
- Is large in size (more than 4-5 centimetres or 2 inches in diameter)
- If there is a suspicion that the tumour could be malignant.
- Adrenal gland cancers (adrenal cortical cancer) are rare tumours that are usually very large at the time of diagnosis. Removal of these tumours is usually done by open adrenal surgery.
If an adrenal tumour is suspected based on symptoms or has been identified by X-ray, the patients are advised to undergo blood and urine tests to determine if the tumour is over-producing hormones. CT scan, nuclear medicine scan, an MRI or selective venous sampling are commonly used to locate the suspected adrenal tumour. Surgical removal of the adrenal gland is the preferred treatment for patients with adrenal tumours that secrete excess hormones and for primary adrenal tutors that appear malignant.
What are the treatment options?
Although laparoscopic Adrenal gland removal has many benefits, it may not be appropriate for some patients. One must obtain a thorough medical evaluation by a surgeon qualified in laparoscopic adrenal gland removal. Aastha is a state-of-art health centre attended by distinguished and experienced surgeons from different fields We have dedicated endocrine surgeons with a great deal of experience with adrenal surgery who are nationally recognized experts in performing and teaching laparoscopic procedures. They are among the most experienced laparoscopic surgeons in the world.
The surgeon may evaluate the patient and suggest either of the two options: Adrenalectomy by laparoscopy or by open incision. Let us see both the options in details:
Open procedure
It is generally accepted that for adrenal cancer and for conditions where there is a high risk of adrenal cancer, such as for large (4-7 cm) tumours or for those associated with multiple endocrine neoplasia, an "open" operation is better because both sides can be examined carefully and dealt with in the event of spread.
The surgeon may operate from any of four directions, depending on the exact problem and the patient's body type. Let us see how the surgeon may approach:
In the posterior approach, the surgeon cuts into the back, just beneath the rib cage. If both glands are to be removed, an incision is made on each side of the body. This approach is the most direct route to the adrenal glands, but it does not provide quite as clear a view of the surrounding structures as the anterior approach.
In the flank approach, the surgeon cuts into the patient's side. This is particularly useful in massively obese patients. If both glands need to be removed, the surgeon must remove one gland, repair the surgical wound, turn the patient onto the other side, and repeat the entire process.
The last approach involves an incision into the chest cavity, either with or without part of the incision into the abdominal cavity. It is used when the surgeon anticipates a very large tumour, or if the surgeon needs to examine or remove nearby structures as well.
Laparoscopic Adrenalectomy
Adrenal glands are two in number and are situated in the abdomen and lie just over each kidney. They produce chemicals that control several important processes in the body. Tumours of the adrenal glands are very rare, and most are non-cancerous (benign) and are treated by an operation to remove the gland called 'Adrenalectomy'. This operation used to be carried out routinely through a long incision in the loin or abdomen (open operation), but is now performed in a considerable proportion of patients through a few small 'keyhole' incisions of 0.5-1.5 cm long.
Laparoscopic surgery refers to the technique in which a surgeon operates within the abdominal cavity with small telescopes and long instruments. Instead of making a large incision which allows the surgeon access to the abdominal contents where he/she operates with conventional instruments and their hands, a series of small (~ 1/4 to 3/4 inch) incisions are made and specialized instruments are used. One of these instruments fills air into the abdominal cavity to blow it up (like a balloon but only under modest pressure). This instillation of air makes it easier to work since the intestines and other organs will fall away from the tissues which are being examined. A camera is then place into the abdominal cavity which allows the surgeon to see what he/she is doing. The remainder of the small holes (ports) have long instruments (forceps, scissors, etc.) placed through them into the abdomen for the actual dissecting of tissues. The patient on the right is positioned on his side for a laparoscopic Adrenalectomy.
Laparoscopic surgery has proved to be a major advancement for the management of adrenal tumours. Patients that have undergone laparoscopic surgery have much shorter hospitalization, more rapid recovery (approximately 2 weeks compared to 4 to 8 weeks after open surgery) and earlier return to work. The postoperative pain is markedly reduced after laparoscopic surgery and the general feeling of physical well being returns at a much faster rate.
We perform the procedure utilizing both standard laparoscopic techniques and with a laparoscopic hand-access device. Two new devices that allow the surgeon to insert a hand inside the abdomen during laparoscopic surgery have recently been developed. The procedure called hand-assisted laparoscopic surgery (HALS) allows better retraction and easier dissection of abdominal organs since the advantages of using the human hand that is present during open surgery is now also available during laparoscopic surgery. We have pioneered HALS techniques for laparoscopic Adrenalectomy and offer this procedure for large tumours in the adrenal gland that otherwise would require an open surgical procedure. We have found the use of the hand assist-device to be advantageous during laparoscopic surgery since the operative time is markedly reduced. Furthermore manipulation of the tumour with surgical instruments is reduced thus decreasing the risk of fracturing the tumour or having an incomplete excision of the tumour. In larger tumours, standard laparoscopic procedures are less desirable, due to the risk of cancer. With hand-assisted laparoscopic surgery large adrenal tumours can be safely removed intact and with a rim of surrounding normal tissue to obtain clean microscopic-free margins around the tumour tissue. Furthermore the ability to intraoperatively palpate the tumour allows the surgeon to make an early assessment as to whether the lesion is benign (non-cancerous) or malignant (cancer) and therefore convert to an open procedure if cancer of the adrenal gland is suspected.
Patient is positioned on the inflatable "bean bag" in the modified flank position (60-70°). We prefer to flex the operative table. The umbilicus can be used as an entrance point, and the camera can be placed in this trocar.· CO2 is insuflated up to a pressure of 18mm/Hg to create pneumoperitoneum. Under laparoscopic guidance, two or three additional working ports are inserted below the rib cage.
Identification of landmarks and trocar insertion.
In a small number of patients the laparoscopic method cannot be performed. In that situation, the operation is converted to an open procedure. Factors that may increase the possibility of choosing or converting to the "open" procedure may include:
- Obesity
-
A history of prior abdominal surgery causing dense scar tissue
- Inability to visualize the adrenal gland clearly
-
Bleeding problems during the operation
- Large tumour size (over 3 or 4 inches in diameter)
The decision to perform the open procedure is a judgment decision made by your surgeon either before or during the actual operation. When the surgeon feels that it is safest to convert the laparoscopic procedure to an open one, these are not a complication, but rather sound surgical judgment. The decision to convert to an open procedure is strictly based on patient safety.
Before the surgery
Most aspects of preparation are the same as in other major operations. In addition, hormone imbalances are often a major challenge. Whenever possible, physicians will try to correct hormone imbalances through medication in the days or weeks before surgery. Adrenal tumours may cause other problems such as hypertension or inadequate potassium in the blood, and these problems also should be resolved if possible before surgery is performed. Therefore, a patient may take specific medicines for days or weeks before surgery.
Most adrenal tumours can be imaged very well with a CT scan or MRI, and benign tumours tend to look different on these tests than do cancerous tumours. Surgeons may order a CT scan, MRI, or scintigraphy (viewing of the location of a tiny amount of radioactive agent) to help locate exactly where the tumour is. The day before surgery, patients will probably have an enema to clear the bowels. In patients with lung problems or clotting problems, physicians may advise special preparations. Some patients may need medications to control the symptoms of the tumour, such as high blood pressure. Drugs such as aspirin, blood thinners, anti-inflammatory medications (arthritis medications) and large doses of Vitamin E will need to be stopped temporarily for several days to a week prior to surgery.
After the surgery
Once the surgery is completed, you will be taken to a post-operative or recovery unit where a nurse will monitor your progress. You will be scheduled for a follow-up appointment two weeks after the procedure. It is important that your bandages be kept clean and dry. Mild discomfort may occur at the incision site so your surgeon may prescribe pain medication. The laparoscopic method results in less pain than the open-procedure method. After the operation, it is important to follow your doctor's instructions. Although many people feel better in just a few days, remember that your body needs time to heal. Post-operative pain is generally mild and patients may require a pain pill or pain medication.
Recovery
Patients are encouraged to engage in light activity while at home after surgery. Patients can remove any dressings and shower the day after the operation. Most patients can resume normal activities within one week, including driving, walking up stairs, light lifting, and work. You should call and schedule a follow-up appointment within 2 weeks after your operation.
In the past, making a large 6 to 12 inch incision in the abdomen, flank, or back was necessary for removal of an adrenal gland tumour. Today, with the technique known as minimally invasive surgery, removal of the adrenal gland (also known as "laparoscopic Adrenalectomy") can be performed through three or four 1/4-1/2 inch incisions. Patients may leave the hospital in one or two days and return to work more quickly than patients recovering from open surgery.
Laparoscopic Adrenalectomy can de performed safely in a cost-effective manner. Given the benefits of this minimally invasive technique, the laparoscopic approach is quickly gaining popularity as the treatment of choice for Adrenalectomy. Results of surgery may vary depending on the type of procedure and the patients overall condition. Common advantages are:
- Less postoperative pain
- Shorter hospital stay
- Quicker return to normal activity
- Improved cosmetic result
- Reduced risk of herniation or wound separation
Complications and risks
As with any operation, there is a risk of a complication. Complications during the operation may include:
- Adverse reaction to general anaesthesia
- High blood pressure
- Bleeding
- Injury to other organs
-
Wound problems, blood clots, heart attacks, and other serious complications are uncommon after laparoscopic Adrenalectomy
For those carefully selected patients who are well-suited for the procedure, people who undergo laparoscopic Adrenalectomy have done much better than those receiving the standard, "open" operations, with a much quicker return to normal activity, a shorter hospital stay, less need for pain medication, and a markedly lower incidence of complications.
If you are really seeking for the Laparoscopic Gallbladder surgery in India, kindly fill up the form for a free consultation by our surgeons. You will be provided with thorough analysis and suggestions regarding Laparoscopic Gallbladder surgery in India you are seeking for. 

















